Disclosure: Some of the links on this site are affiliate links. This means that if you click on the link and purchase an item, I may receive a small commission at no extra cost to you. I only recommend products and services that I personally use, trust, or believe will provide value.
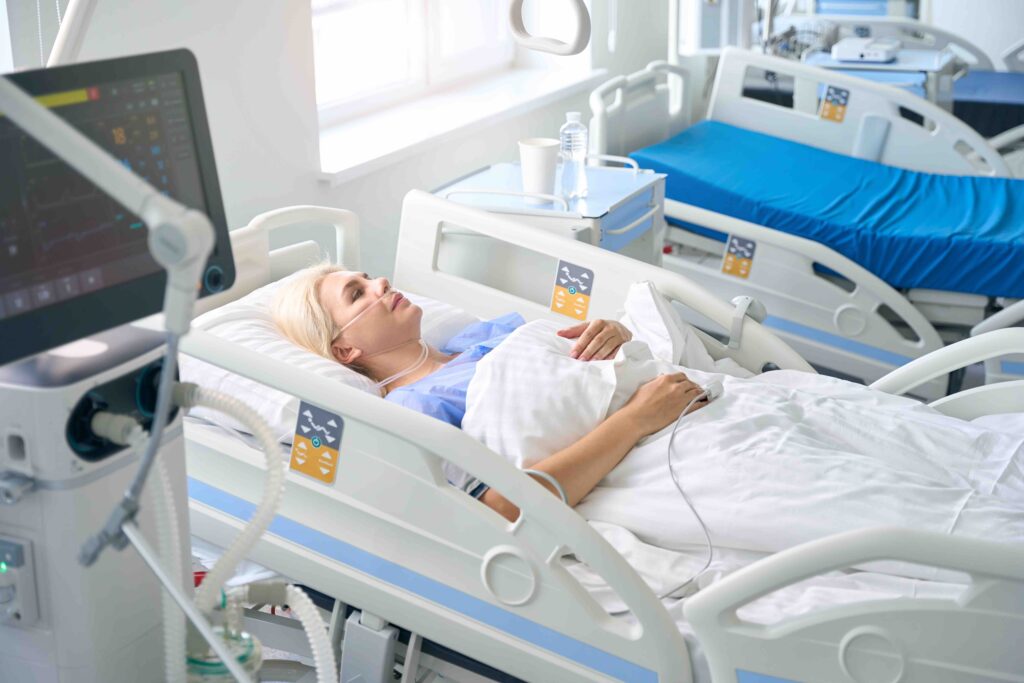
What Does a PACU and Pre-Op Nurse Do?
As a nurse working in the surgery setting, I work both in Pre-Op and PACU.
In Pre-Op, my role is to make sure the patient is surgery ready. I confirm appropriate consents, check NPO status, review medications, start IVs, and give pre-anesthesia medications.
In PACU, I receive patients coming out of surgery from the OR. I focus on keeping them comfortable and managing pain, nausea, and other symptoms as they wake up.
I’ve worked in both an Ambulatory Surgery Center (ASC) and a hospital-based inpatient surgery setting. There are a lot of similarities, but the difference can honestly feel night and day.
In outpatient settings, most cases are elective, so patients are generally healthier and have fewer complex comorbid conditions compared to hospital-based inpatient surgery.
I really enjoy working in an ASC. It’s one of the easiest nursing jobs I’ve had, and I feel very thankful that I accidentally found this specialty. It genuinely helped improve my mental health as a nurse.
The lifestyle as a Pre-Op and PACU nurse is also great. There are different scheduling options that can fit your life. Most ASCs have a Monday to Friday schedule with 8-hour shifts, similar to clinic hours, while hospital-based inpatient surgery usually have longer shifts of 10 to 12 hours per day, typically 3 to 4 days a week.
I personally prefer longer shifts and working fewer days.
Meanwhile, the workflow in both outpatient and inpatient surgery settings is manageable, and most of the time I feel like I actually have enough time to fully focus on my patients.
Read: Is Per Diem Nursing Right for You?
What PACU and Pre-Op Nursing Actually Looks Like

Pre-Op
Pre-Op is fast-paced and structured.
The OR schedule is usually set days or even weeks in advance. Patients are instructed to arrive about 2 hours before their scheduled surgery.
In Pre-Op, we:
- confirm patient identifiers
- verify correct consents and sometimes obtain them
- check vital signs and report anything outside baseline
- interview the patient regarding NPO status, recent illness, implants
- review medications
- start IVs and give pre-anesthesia meds
PACU
In PACU, we:
- receive the patient from the OR
- get report from the OR nurse, CRNA, or anesthesiologist
- obtain initial vital signs
- ensure patient comfort
- manage symptoms like pain and nausea
- prepare the patient for discharge
At both Pre-Op and PACU, we typically care for a maximum of 1 to 2 patients at a time, which is a huge difference compared to the usual 4 to 5 patients in inpatient bedside settings such as Med-Surg, telemetry, and other units.
Types of Cases
This depends on the facility.
In ASC settings, cases are usually more straightforward:
- cataract surgeries
- minor orthopedic procedures like carpal tunnel
In hospital-based inpatient surgery settings, you’ll see more complex cases:
- appendectomies
- nephrectomies
- joint replacements
I’ve worked in both environments, and honestly, I wish I could have stayed in ASC. I only moved back to an inpatient surgery setting because my new PACU position offered a better commute, healthcare benefits, and better hours.
Even with that change, I still prefer Pre-Op and PACU over any other specialty I’ve worked in.

Why I Love PACU and Pre-Op Nursing

1. Better Work-Life Balance
This is one of the biggest reasons.
One of the best things about nursing is the flexibility in scheduling, and PACU/Pre-Op really highlights that.
If you prefer a traditional schedule, many outpatient settings run Monday to Friday clinic hours.
Personally, I don’t enjoy that schedule. I prefer longer shifts with fewer workdays.
My ideal schedule, which I finally found after constantly stalking my workplace’s career website. Now I work my dream schedule of 10 hour shifts, 2-3 days/week.
That gives me time to do other things I enjoy outside of nursing like writing, working on my website, and most specially spending time with my family.
I also have coworkers who prefer 3 twelve-hour shifts, which works well for them too.
2. Generally Healthier Patients

This is the key phrase: healthier patients.
This is especially true in ambulatory surgery settings, but even in inpatient surgery settings, anesthesia teams are very cautious when it comes to high-risk patients and will thoroughly assess whether it is safe to proceed with surgery.
Many critically ill patients go straight to ICU instead of PACU.
Because of this, it’s relatively uncommon to manage highly complex medical cases in PACU.
3. Lower Stress Compared to Bedside

I’m not going to lie.
Every time I give report to an inpatient nurse, especially in a Med-Surg unit, I feel a little bad.
I know they might already have multiple patients, possibly another admission coming from the ER, and several patients requiring a lot of attention.
Meanwhile, in PACU, I usually have one patient, sometimes two.
That’s why I make it a point to manage pain and symptoms as much as possible before sending the patient up.
I often tell patients: “Let me take care of it now because your nurse will be very busy upstairs.”
I explain that once they leave PACU, their nurse in Med Surg will have several other patients and probably less time to focus on them.
4. Care Is Focused on Immediate Needs
In PACU, we are very focused on immediate post-operative symptoms.
We manage:
- pain
- nausea
- blood pressure
We are not managing chronic conditions or long-term care plans.
Even if patients have scheduled medications, many of those are not immediately necessary in PACU and can be given later on the inpatient unit.
Also, in my almost 7 years in PACU, I have never had to call for a psych consult or social work for complex psychosocial issues.
5. More Control and Autonomy
One of the best parts of working in Pre-Op and PACU is having standing orders.
Most of the medications you need are already ordered, so you don’t have to constantly page a physician.
In Pre-Op, medications are very routine.
In PACU, there are standard protocols for pain and nausea management.
We also work closely with anesthesia, who are usually readily available.
And honestly… you never have to page a doctor in the middle of the night for something like Colace.
6. Healthier Work Environment
Because the workload is more manageable, it reflects in the work culture.
In both outpatient and inpatient surgery settings, PACU staff tend to be:
- less stressed
- less toxic
- more supportive
There’s generally more teamwork and camaraderie.
7. Routine, But Still Different Every Day
There is definitely a routine, especially in Pre-Op where you follow similar steps for every patient.
In PACU, you also see similar types of cases depending on the specialty of the surgery center.
For me, routine is actually a good thing. It helps you become efficient, and the workflow becomes second nature.
But it’s not boring because you still get different patients every day.
Unlike inpatient bedside settings where you might have the same patient for multiple shifts or days, sometimes with very challenging situations.
8. Minimal to No Shift Report
Shift report used to be one of the most stressful parts of inpatient bedside nursing for me.
I tend to be a people pleaser and conflict-avoidant, so I would try to finish everything just to avoid any tension during report.
In PACU, you admit the patient, recover them, and discharge them.
That’s it.
No long reports. No back-and-forth or passive-aggressive issues with the next shift.
9. You Actually See Patients Get Better

This is probably one of my favorite parts.
You see patients come in for a specific problem, go through surgery, recover, and then most go home feeling better.
It’s a short but meaningful interaction.
Most of the time, patients leave happy and thankful, and you get to end your interaction on a positive note.
10. No Endless Discharge Barriers
In inpatient bedside settings, discharge can be complicated.
You’re dealing with:
- placement issues
- family situations
- complicated financial issues
Sometimes patients stay for extended periods because of these barriers.
In PACU, it’s much simpler.
Patients either go home or get transferred to inpatient units.
11. A Softer Version of Bedside Nursing
I hear a lot of nurses want to leave bedside completely, and I get it.
Even though I work in an inpatient surgery setting, working in PACU and Pre-Op still feels like a softer version of bedside nursing.
You still use and maintain your clinical skills, but without the same level of stress and workload.
The Reality: It’s Not Perfect
It’s not all perfect.
There is increasing pressure to move patients faster, I hear its because OR time is expensive. Don’t really know.
Sometimes surgeons or OR staff push for quicker turnover, which can feel rushed.
In PACU, there are times when surgeons want patients discharged within a specific timeframe, even when they may not be fully ready.
Pre-Op can also feel repetitive, and in outpatient settings, some skills may not be used as often.
Also, patients are often anxious in Pre-Op and may need a lot of reassurance.
In PACU, not all patients wake up comfortably. Some wake up in pain or distress, and you need to be ready to manage that right away.
Who Should Consider PACU or Pre-Op Nursing
This is a great option for nurses who:
- are feeling burned out from inpatient bedside settings
- want better work-life balance
- prefer caring for 1 to 2 patients at a time
- want to focus on immediate patient needs
PACU can be difficult to get into, and most positions require at least 1 to 2 years of critical care experience, but it is definitely worth considering.
Final Thoughts: Why I’m Staying in PACU
Being a PACU nurse honestly changed my life.
About 10 years ago, I was burned out working in ICU and could easily have been one of those nurses posting R/Nursing about how much they hated nursing.
But PACU helped me enjoy being a nurse again.
At this point in my life, I’m not looking for the intensity of ICU or the constant demands of inpatient bedside care.
What matters more to me now is having the time and energy to enjoy life outside of work.
And PACU allows me to do that.
FAQ
Is PACU nursing stressful?
When I worked inpatient, I needed anxiety medication just to sleep after my shifts, even though I was exhausted from working a 12-hour shift.
Thank God, I don’t have that issue anymore.
I sleep well, and my pre-shift anxiety is gone.
Do PACU nurses make more?
In my experience, pay is similar to ICU and other specialties. Sometimes even slightly higher since it is considered a specialty.
Is PACU a good job for new grads?
I wouldn’t recommend it for new grads.
You need strong assessment skills and the ability to recognize a rapidly deteriorating patient. Most PACU roles require prior critical care experience.